FUNDRAISING FOR A CURE
Donating is simple, fast and totally secure. Your details are safe with us and we will never sell them
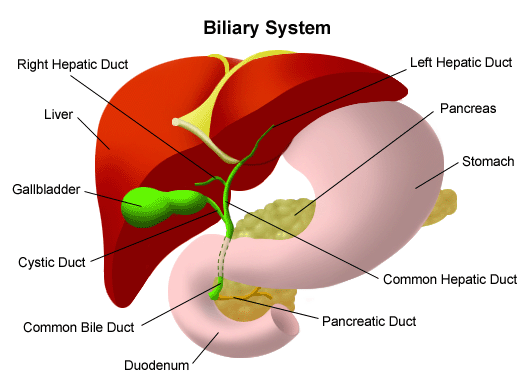
Liver & Biliary Tumours
The liver is a large organ which lies in the upper part of the abdominal cavity, directly beneath the diaphragm. The functions of the liver are very complex, but they can basically be considered in four key areas: protein formation, production of bile, sugar metabolism and breakdown of waste products and toxins from the blood stream. A healthy, functioning liver is essential for life.
Common symptoms
Many liver diseases have no symptoms at all apart from making you feel a bit run down.
Jaundice is a yellow pigmentation of the eyes and skin, which occurs when there is a build up of bilirubin (a constituent of bile) in the blood stream. If this is caused by a blockage to the outflow of bile from the liver (obstructive jaundice) then this may be associated with itching of the skin as well as very dark urine and pale faeces. Jaundice may also be caused by inflammation or infection of the liver (hepatitis) as well as by cirrhosis, excessive breakdown of red blood cells (haemolysis) and a large number of other complex metabolic conditions.
Some conditions affecting the liver are painful; pain from the liver is usually felt in the top right hand side of the abdomen, just beneath the ribs, it may be worse on taking in a deep breath. The pain may also be felt to travel or radiate around to the back or right shoulder. Similar pains can come from the gallbladder, diaphragm, spine and chest which can make liver pain hard for doctors to diagnose.
Fluid retention can occur in some liver disease such as cirrhosis. This usually takes the form of swelling of the abdomen (tummy) and ankles.
Bruising of the skin can occur if the liver is not making clotting factor proteins properly.
Encephalopathy is a term used by doctors to describe the drowsiness and confusion that can occur in patients with liver failure, it is also quite common for a few days after major liver surgery. It is caused by a build up of waste products in the blood stream in particular ammonia.
Hepatitis and cirrhosis of the liver
Hepatitis is inflammation of the liver; it may be caused by a number of conditions including infections (such as viral hepatitis A, B or C), chemicals (e.g. alcohol), drugs (e.g. paracetamol overdose) or disorders of the immune system.
When there has been longstanding inflammation of the liver, it develops areas of chronic scarring and fibrous tissue around patches of regenerating liver cells. This pattern of scarring (fibrosis) and regeneration is the start of cirrhosis of the liver.
Treatment of both hepatitis and cirrhosis is aimed at finding the cause of the inflammation and treating or stopping this first to prevent more permanent damage occurring. Surgery is reserved for managing the complications of cirrhosis. Liver transplants are performed at a small number of centres across the UK for very specific circumstances in patients with advanced cirrhosis or severe liver failure from a variety of causes. We do not perform transplants in Southampton, the nearest large centres are London (King’s), Birmingham (Queen Elizabeth) and Cambridge.
Benign liver disease and tumours
There are many dozens of benign (i.e. not cancerous) conditions that affect the liver, most of them do not require any treatment once we are sure of the diagnosis. Here are a few of the ones that we as liver surgeons are most often asked about by patients.
Haemangiomas are benign liver lesions that are virtually always harmless. They are very common and are caused by an overgrowth of blood vessels at one or more sites in the liver. They are often picked up on scans of the liver, but even very large haemangiomas do not usually require any treatment or cause any symptoms. Rarely they can appear similar to more worrying tumours on scans and under these circumstances we occasionally perform surgery to remove one to confirm that this is the correct diagnosis. However usually the appearances on scans are sufficient to confirm the diagnosis
Liver cysts are rounded collections of fluid within the liver, they are benign, very common and nearly always harmless. Very large cysts may become uncomfortable if they stretch the liver or press on adjacent organs such as the diaphragm, stomach or bowel. Massive cysts can reach diameters of 20-30 cm (8-12 inches) and contain several litres of fluid, cysts of this size may give a visible swelling in the abdomen (tummy) and be very uncomfortable, often associated with pressure symptoms which may include shortness of breath from pressure on the diaphragm.
A few people have rare polycystic conditions affecting the liver where the liver is full of hundreds of small and large cysts. Sometimes these are associated with cysts in other organs such as the kidney.
If there has been haemorrhage (bleeding) or infection or inflammation in the cyst then the fluid inside it may become thickened and form strands of internal scar tissue, these can make the cyst look like a more complex lesion such as cystadenoma (see below). Appearances are even more hard to interpret if there has been infection in the cysts as well.
Patients with bad pressure symptoms from large cysts often benefit from keyhole surgery to drain and de-roof the cysts and improve their discomfort, this is usually a very effective treatment, particularly for patients with large solitary cysts.
For patients with large numbers of small cysts surgery is less effective and therefore surgery may not be advisable unless we think that we can effectively deal with a particularly dominant cyst or prominent cluster of cysts that appear likely to be contributing to your symptoms.
Focal Nodular Hyperplasia (FNH) is an uncommon benign condition that affects the liver mainly in young and middle aged women. It does not usually cause any symptoms. The main difficulty with this condition is that it can look similar to some other more serious liver problems so we often investigate it more extensively and very occasionally biopsy it or remove the area surgically to be sure that it is safe. Rarely very large areas of FNH can compress adjacent organs or structures inside the tummy and cause symptoms such as heart burn or indigestion after eating, under these circumstances keyhole surgery may be offered to remove the tumour.
Liver adenoma is a rare benign tumour of liver cells; it occurs more often in women and is sometimes associated with oestrogen treatments such as the contraceptive pill or HRT. They can also be related to other steroid hormone treatments and drugs, including anabolic steroids used in body building. We frequently operate and remove adenomas as there is a small but significant risk that they can rupture and bleed heavily, a small number may also turn cancerous in the long term. Some small adenomas may regress and disappear if oestrogen treatments are stopped, although this phenomenon is well reported in the medical literature it is rarely seen in clinical practice hence we usually end up removing these tumours, often as a keyhole operation.
If the tumours bleed we often embolise them (see below) to block off the bleeding blood vessel, before removing the tumour at a later date.
Multiple adenomas (or adenomata) arising simultaneously in a patient are most commonly related to hormone treatments. Large or symptomatic tumours are usually removed and smaller ones embolised, we will follow you up long term if you have had this pattern of liver disease. Very rarely liver transplant has been required for patients with multiple adenomata.
Cystadenoma is a very rare benign tumour often affecting the central portions of the liver, these tumours also have the tendency to turn cancerous in the long term and we usually operate and remove them. It can be difficult to diagnose this condition which can appear similar to other cystic liver diseases such as hydatid disease or simple liver cysts.
Hydatid disease is a disease caused by a parasitic infection. It is rare in the UK but common in many parts of the world, particularly in areas where sheep farming is prevalent. The parasite (echinococcus) has a complicated life cycle involving sheep (or goats), dogs and occasionally man. The parasites grow in cysts in the liver and may have no symptoms or they may cause pain, fever, abdominal swelling or jaundice. The parasitic infection is usually treated initially with several months of antiparasitic medication (e.g. albendazole), to eradicate the most active disease, followed by surgical resection of the cysts. The prognosis is excellent if caught early and correctly treated.
Necrotic nodule is a term used to describe areas of dead liver that have formed hard shrunken areas of scar tissue, sometimes they are thought to represent dead tumours that have outgrown their blood supply and shrivelled up, they may also arise in areas of previous liver injury. The precise reason why they occur is not usually known. They are of no consequence in themselves, however they are very hard to diagnose and often look suspicious on scans hence again they may be removed if we find them whilst investigating the liver.
Angiomyolipomata are fatty tumours made of fat, fibrous and muscle cells with a very rich blood supply. They are rare in the liver but occur much more frequently in the kidney. Occasionally patients have large numbers of these replacing the normal liver tissue in a similar way to polycystic liver disease can. Normally liver function is preserved, but the enlarged liver can cause pressure symptoms or upper abdominal discomfort.
Peliosis is an extremely rare condition affecting the liver in which a fast growing knot of blood vessels develops within the liver. It is most likely to occur during pregnancy and can cause heavy bleeding. It is best treated by embolisation (see below) which can be curative.
Primary Malignant tumours of the liver
Liver cancers fall into two broad groups: primary cancers which have arisen in the liver and secondary cancers which have spread to the liver from another organ.
Anyone with primary liver cancer should have their condition assessed by a specialist multi disciplinary team (MDT) including at least one hepatologist (liver doctor), oncologist (chemotherapy cancer specialist), hepatobiliary radiologist (liver X-ray / imaging specialist), hepatobiliary pathologist and a liver surgeon, before deciding on treatment. The only centre on the South Coast with all of these specialists is Southampton. Patients with secondary liver cancers from bowel cancer, neuroendocrine tumours, kidney cancer and GIST cancers should also all be assessed by a liver MDT.
Hepatocellular carcinoma (HCC or hepatoma)
HCC is a primary liver cancer. It is much more likely to occur in people who have cirrhosis, particularly if it is associated with hepatitis B or C infection or haemachromatosis (a rare metabolic disorder). Small HCC’s usually do not give any symptoms, but larger tumours often give upper abdominal discomfort and may be associated with signs of liver failure such as jaundice, drowsiness and fluid retention. They occasionally cause intra abdominal bleeding.
Treatment may be with surgical resection, liver transplant, radio-frequency ablation (RFA) or trans arterial chemo embolisation (TACE). The treatment that we use depends on the quality of the background liver (i.e. cirrhotic or healthy) the site and size of the tumour and the relationship of the tumour to the major blood vessels in the liver. Small tumours are usually straightforward to treat. Large tumours can be much more problematic, particularly if they are in the centre of the liver or involve major blood vessels.
Patients sometimes present with several small HCC tumours dotted around the liver, in these cases a combination of treatments may be used, using TACE to shrink the bigger tumours, RFA to treat central liver tumours and surgery to remove more accessible, superficial deposits of disease.
Although traditional chemotherapy has not been very helpful in HCC in the past, there are some new chemo drugs that are becoming available which appear to be much more effective in controlling this type of cancer. In particular Sorafenib a tyrosine kinase inhibitor appears to work well in some people with this tumour. We hope that they will prove to be a powerful additional treatment to complement surgical and radiological techniques. For further advice on this you would need to speak to an oncologist (chemo specialist).
Cholangiocarcinoma
This is an uncommon primary malignant tumour (cancer) of the bile ducts, which can arise in the small bile ducts within the liver, the big branches in the centre of the liver (hilum) or in the main bile duct draining out of the liver. It is increasing in frequency in the UK for reasons that are not fully understood. It is more common in patients who have had tropical parasitic infestations of the bile ducts (clonorchis), originate from north west asia (Afghanistan / Pakistan / north west India) or have had sclerosing cholangitis (chronic inflammation of the bile ducts).
Cholangiocarcinomas are difficult to treat because they often arise in the centre of the liver and involve the main blood vessels and bile ducts entering and exiting the liver at this point. Bile duct tumours in this central part of the liver are called hilar cholangiocarcinomas (or Klatskin tumours). Approximately 20% of patients with hilar cholangiocarcinoma are suitable for surgical resection of the tumour. The operations are often more extensive than routine liver resections and usually involve major liver resection as well as removal of the bile duct and wide clearance of lymph glands around the liver to try and clear the tumour. Sometimes it is necessary to divide and reconstruct the blood vessels entering the liver (portal vein or hepatic artery). This is amongst the most difficult surgery that we perform. Bile duct tumours that arise more peripherally on the edge of the liver are a little easier to treat, although the principles are the same.
Bile duct cancers arising in the bottom end of the bile duct (in or near the pancreas) do not need liver surgery but are best managed with major pancreatic operations (Whipple’s procedure – see pancreatic surgery section).
Gallbladder cancer is another type of cholangiocarcinoma (see above) which develops inside the gallbladder. It often spreads directly into the liver and often blocks off the bile duct and blood vessels in the centre of the liver. Large tumours present the same difficulties as hilar cholangiocarcinoma (see above) and are managed in an identical fashion, however sometimes gallbladder cancer is caught at a very early stage, when the outlook and management strategy is rather different.
Small, early gallbladder cancers can be very hard to identify and often have similar symptoms to gallstones with upper abdominal pain related to eating fatty foods. On scans it can be difficult to be sure if the problem is a benign polyp, unusual gallstone, gallbladder scarring / inflammation or a small cancer. In this case where there is diagnostic doubt and a suspicion of a tumour, then we usually recommend a keyhole operation under general anaesthetic, inspecting the gallbladder with a laparoscope to see if it looks cancerous and then removing it intact, often with a small block of liver tissue and the adjacent lymph glands to ensure that it is all taken away. This is sent for analysis, if cancer is confirmed then for early tumours no other treatment is necessary. However sometimes further open surgery may be required if the tumour is invading more deeply into the liver or lymph nodes.
Unfortunately the commonest scenario that we encounter is that the tumour has been found by chance in someone who has had their gallbladder removed for painful gallstones, the patient is then referred on to us for a specialist opinion and further treatment. This is not absolutely ideal as it is best to remove early gallbladder tumours with some surrounding tissue to ensure clearance of all the disease, however it is often not possible to identify these tumours beforehand. Under these circumstances we usually try to perform further keyhole surgery to remove tissue from the liver next to where the gallbladder was, the stump of the cystic duct (the connection of the gallbladder to the bile duct) and the lymph glands nearby. We also remove a core of skin and scar tissue from the old port sites where the gallbladder was previously removed. If all of this tissue is clear no further surgical treatment is necessary. If tumour is found to infiltrate widely into the areas that we have removed then more extensive open surgery as for hilar cholangiocarcinoma is required.
Secondary Liver Cancers
Until the last twenty years almost all secondary cancers in the liver were considered inoperable. As surgical techniques have improved and our knowledge of the behaviour of different types of cancer has expanded the indications for operating on secondary liver cancers have widened. New chemotherapy drugs that can shrink tumours have also helped to broaden the number of cases that we can offer surgery to.
Colo-rectal cancer secondaries
The most common secondary cancer that we operate on after it has spread to the liver is bowel cancer (colon and rectum cancers). Approximately 30-40 per cent of all patients with spread of this tumour to the liver are operable. Due to the more favourable nature of this cancer it is even sometimes possible to manage spread to the lung with surgery as well (in conjunction with our colleagues in the chest surgery unit). The risks of liver surgery to the patient are relatively low with approximately a 1 in 100 risk of death whilst in hospital for healthy patients undergoing conventional liver surgery. High risk patients (e.g. very elderly or with severe heart or lung disease such as angina or emphysema) and more extensive resections can have a much higher risk.
Out of the patients that we operate on for bowel cancer secondaries (metastases), most will have a significantly prolonged life span and between a third and a half of all the patients that we treat are cured of their cancer. Without surgery the disease is effectively incurable, although chemotherapy may substantially improve the length of survival for many patients. The best results are seen in patients who are able to have a combination of liver surgery and chemo. If you have been on a standard chemo regime we usually suggest waiting for approximately 4 weeks after your last cycle of chemo treatment before having surgery to allow you and your liver to recover before the operation. If you have had a more intensive chemo regime with some of the aggressive new drugs that are available we might suggest waiting for 8 or more weeks to allow you and your liver to recover before facing the surgery.
The decision about whether surgery is the right treatment needs to be made by a multidisciplinary team involving a specialist liver surgeon, chemotherapy expert (oncologist), radiologist (X-ray imaging doctor) and other interested professionals. As our expertise in this field has increased we have been able to successfully operate on more complicated patterns of disease. The number of tumours and their size does not make greatly influence our ability to operate. We have removed more than 20 tumours at a single operation and individual tumours over 25cm (10 inches) in diameter. The important question is not so much what needs to be removed, but rather how much healthy liver can we leave behind. If we can remove all the disease and leave enough good liver behind then the operation is possible.
Sometimes in patients with several tumours involving both sides of the liver we see a pattern of disease that means there are too many tumours to safely treat in one operation, under these circumstances we may do a two stage operation. This usually involves operating on one side of the liver first (usually the left side, often as a keyhole operation) to clear the cancers from this side and let it grow back before operating on the other side a few weeks later.
If we think that the tumours are placed directly on the important blood vessels entering or leaving the liver then surgery may be very high risk or not possible and other treatments may be necessary. There are few absolute rules under these circumstances and each of these difficult or high risk cases must be carefully weighed up by the whole team to offer the patient the best options.
Neuroendocrine tumours (NET or Carcinoid tumours, for more detail follow the link to the NET section of the PLANETS website)
These are tumours that grow from hormone secreting cells in the digestive tract. They can arise almost anywhere in the intestines and related digestive organs and subsequently spread to the liver. They have a very wide range of clinical behaviour, some tumours are small, slow growing and almost benign in nature, at the other end of the spectrum there are very fast growing aggressive forms of the disease that behave in a similar manner to the more common bowel cancers. Most tumours behave somewhere between these two extremes. Many of these tumours produce hormones that can produce classic symptoms when the hormones are released from the tumour into the blood stream such as:
- serotonin (5-HT), most commonly released from “mid gut” tumours arising from the small intestine, appendix or right side of colon, tumours secreting this hormone produce the classic carcinoid syndrome of facial and body flushing, palpitations (racing heart beat), dizziness and occasionally wheezing, shortness of breath diarrhoea and cramping abdominal pains. These symptoms may be triggered by stress, exertion, certain foods and alcohol.
- insulin, one of the hormones made by the pancreas to control blood sugar levels. It acts to lower blood sugar in response to the normal fuctuations that follow a meal. In insulinoma (a variety of NET arising from the pancreas) excessive amounts of insulin are produced with a tendency to develop very low blood sugar levels, this may lead to dizzy spells and cravings for sweet foods.
- glucagon, another blood sugar regulating hormone that has the opposite action to insulin producing a higher blood sugar. This results in fatigue, weight loss and in some cases a diabetes type picture.
There are many other types of hormones that these tumours can produce including gastrin (which gives peptic ulcers), Pancreatic Polypeptide and VIP, which can give profuse watery diarrhoea.
The tumours can be hard to diagnose initially as they grow in parts of the abdomen that are hard to assess clinically and because the symptoms are often slowly progressive over several years they are often misdiagnosed as irritable bowel syndrome, gallstones, menopause symptoms, panic attacks or crohn’s disease before the true diagnosis becomes evident. The classic sites for the primary to occur in are the pancreas, small intestine and appendix, but they can arise anywhere from the gullet to the rectum. Liver secondaries are often manageable by surgery, although it is difficult to cure these tumours it is often possible to extend and improve life by many years through a combination of surgery and other medical and radiological treatments.
In Southampton we have a dedicated carcinoid Multi-Disciplinary Team, including surgeons, nurses, radiologists, oncologists, nuclear medicine specialists, anaesthetists gastro-enterologists and endocrine physicians. Between us we assess each case and decide on the correct course of management to cure or treat the tumour. We run a joint clinic every fortnight and have a video-conference meeting with our colleagues from around the region where we can discuss new patients together and advise on investigations and management.
The traditional approach to these tumours has been to “watch and wait”, treat the symptoms as they arise and only operate as a last resort. However advances in the treatments we can offer mean that this traditional palliative approach is no longer advisable or acceptable for most patients, since it makes little difference to length of survival, no chance of cure.
Our philosophy is to treat the disease aggressively as soon as we can to reduce the number of viable cancer cells left (sometimes called cyto-reduction) to a minimum using whatever are the most effective treatments we have available. This multi-modality cyto-reductive strategy offers the patient the best long term chance of disease control, symptom control and prolonged survival.
Gastro Intestinal Stromal Tumours (GIST / Leiomyosarcoma)
These are rare cancerous tumours usually arising from the muscular wall of the stomach or intestines. They frequently spread to the liver and very good results can be achieved by a combination of surgery and new chemotherapy agents, particularly glivec (imatinib) and sutent (sunitinib), these drugs are from a family of agents called tyrosine kinase inhibitors, they work by stopping the cells from growing and effectively making the tumours dormant.
The key decisions in these tumours relate to their size, position, biological behaviour and response to chemo. All of these factors influence the timing of surgery to remove them. Small tumours should be removed surgically at the earliest opportunity, large tumours involving several organs should be treated with glivec first to shrink them and then surgically removed after peak response to the chemo has been achieved. This is usually after about 6 to 9 months.
Other Tumours
The largest series of data from the world’s biggest liver surgery centres have reported successful results from liver surgery for a wide variety of other secondary cancers. Almost all of these cases are highly selected individual patients who have favourable patterns of tumour behaviour and spread that make resection appropriate. Our own combined experience of over 600 liver resections supports this highly selective practice for a few patients with liver secondaries from the following cancers.
Occasionally
Malignant melanoma (skin cancer, arising from pigment cells)
Ocular melanoma (melanoma cancer arising within the eye)
Renal (kidney) cancers
Adrenal cancers
Rarely
Gastric (stomach) cancers
Breast cancer
Very rarely
Testicular teratoma
Thyroid cancers
Sarcomas
Oesophageal (gullet) cancers
Lung cancer (Adenocarcinoma variant)
Subscribe to our Newsletter
Get informed about the latest news straight to your inbox